|
7/29/2013 Beautiful Compensations of Caring"It is one of the most beautiful compensations of life, that no man can sincerely try to help another without helping himself."  Throughout my life, I have come to know a deep spiritual truth: We are all connected. According to Chief Seattle, "Humankind has not woven the web of life. We are but one thread within it. Whatever we do to the web, we do to ourselves. All things are bound together, All things connect". To me, this connection called the web of life means that every action we take (or avoid taking) has an impact somewhere, either within our own lives, on other life forms, or upon our environment. This idea has been reiterated by many wise poets, writers, philosophers and theologians, so it is not new. However, I think it applies even more strongly to the relationship of caregiver to care receiver. I'm speaking here of the quality of our caregiving experience, from both sides of the equation. I've written in this blog of some of the negative consequences caregiving can have, in terms of the caregiver's health, happiness and sense of balance in life. All true. But I want to give some time also to the beautiful compensations, those incredibly precious moments of connection at the soul level, that can be a part of caregiving as well. Every person and situation is as unique as a fingerprint or snowflake, so generalizing is risky. But I think this is a crucial part of creating a more serene, beneficial experience, so I am willing to go out on this limb. In caring for my mother, I learned (sometimes the hard way!) that we were incredibly connected -- whether that was judged a good or bad thing was up to me and the perspective I chose. She responded to me on an almost psychic level at times, picking up on emotions and reactions of which I might be totally unaware. She often understood that something was upsetting me, even before I knew it! Though she could not always ferret out the correct reasons, she still related to me from this knowing. I soon realized I could not "fool" her into believing everything was fine if it wasn't. So, I had to clear my own mind and heart before approaching her. I could not hide behind a pretense or falseness. Mom spotted that immediately! She was like a dolphin whose echo-location scanned below the surface, all the way through my innermost self, and saw truth. It reminded me of times as a child when I believed Mom could tell if I was fibbing by looking into my eyes. Perhaps she could -- a mother's own type of radar or a truth-seeking missile. There were several activities we did to nurture and connect us: music was a powerful device for this. We often sang together, watched musicals on DVD that were her favorites, and listened to hymns or songs by Nat King Cole, Bing Crosby, and other "crooners" from Mom's era. I wish that I'd known about the iPod Project (www.musicandmemory.org and on this site click here) in time to use that with my Mom. But, alas, I learned of it too late. Another connection was found through flowers, specifically roses -- that lovely flower was Mom's talisman, since she grew a beautiful rose garden which she shared with her friends to uplift and bless them all her life, so it was perfect for reminiscing. And, lastly, perhaps the most potent of all: simple loving touch. I used gentle, soothing touch with Mom every day -- putting lotion on her skin, gently rubbing her back at bedtime, using aromatherapy oils on her hands and arms, hugging her several times a day, touching her arm or hand as we walked, reaching over to pat her knee as we watched TV or in the car. I used touch along with giving her reassuring words, and loving eye contact. It was this that most often sparked a spontaneous "I love you", or "You're a little sweetheart" (her favorite term of endearment). Now, in the interest of being completely candid, I must report that I am not a saint. There were days when exhaustion, lack of sleep, worries, distractions, stress or any number of other things got in the way of my being the best caregiver I could be. There were days I didn't much like myself for being tired, short-tempered, upset. I've had to figure out how to forgive myself for not being perfect, for not always knowing how to approach this huge job of being completely responsible for another life. Most days I can do that. I'm still working on it. I wanted to share this, from my heart, because I know that the one thing caregivers often find in short supply is hope. Hope for a loving positive experience in caring for one they love. My advice is to create that hope and joy one moment at a time. Make this moment count. Use all your creativity and passion to connect through all the senses -- sound, touch, smell, sight and taste. Be present as a healing, loving being right now. Let the next moments and days take care of themselves as much as you can. And find the peace and grace of those beautiful compensations of caring -- one moment at a time. 12/26/2012 Being Alive Inside: Music & Memory"If music is such an important aspect of people's lives from the time they are born, why is it that it doesn't really occur to us, as a society, to provide people with music when they can no longer do what is necessary to provide it for themselves? Imagine: You are lost in a world where words no longer make sense, when you only dimly know the faces around you, if at all (including beloved family members), and indeed where you may not remember your own past at all. Your entire world has shrunk down to a dim, lonely place behind a dark curtain of dementia or depression. Then, someone approaches you with a smile and friendly manner and places headphones on your ears and begins playing a song that you danced to with your sweetheart at your wedding. The music immediately connects you to that pleasant past memory, to who you were at that time, forming an acoustic bridge that can span what words or touch may no longer be able to do. Your eyes brighten, your toes tap, your lips curve in a smile and the words to the song come out of your mouth, which had forgotten how to speak. The light in your soul begins to peek out from behind the dark curtain. You may even kick aside your walker and do a little dance. Is this fiction or fact? Well, in a 2008 project which provided 200 ipods to residents in four nursing homes in New York, it is fact. And Dan Cohen, then man behind the project and founder of Music and Memory, is seeking to make it fact for millions more! Mr. Cohen has pioneered the program Music and Memory with the goal of making personalized music the standard of care at all 16,000 nursing home facilities around the country. If the viral Youtube clip of Henry, a 94-year-old nursing home patient who is transformed in an astonishing "awakening" to the music on the provided ipod, is any indication, this is an idea whose time has most definitely come! Mr. Cohen is using the power of the media to bring this transformative technology to all the elder care advocates, nursing homes, family caregivers, and others who can use it to transform sadness and isolation to toe-tapping joy and song with the implementation of a personalized playlist for people with dementia. Cohen and his team are at work on a documentary (Alive Inside - www.aliveinsidemovie.com) which features Henry and many others whose lives have been returned to them in part, by this power of their musical past and its impact on the brain. Music and Memory and the Alive Inside documentary have been featured on numerous media, such as NPR, New York Times, USA Today, CNN, MSNBC, ABC, and The Doctors, and have completed a successful campaign on crowdsource funding site Kickstarter. Speaking as a daughter, a singer, and a caregiver, this is the most wonderful use possible of the gift of music to help our loved ones reconnect to their past, to bring them joy in the present, to make their lives so much richer and happier -- and all for the price of an ipod and some tunes and a caring person to put them together. The Music and Memory website has a wealth of resource material to allow you to get involved at whatever level you choose -- from how to set up a playlist for a loved one with Alzheimer's at home, to running a donation drive for gently used iPods which they will refurbish for use in nursing homes. Donate in whatever way feels right to you -- as a volunteer, by giving an old iPod to the cause, with financial support, and by spreading the word (and the music) on your social media such as facebook and twitter. This is a chance to positively affect literally millions of lives. Don't miss out! 10/3/2012 Memory Cafes & Overnight Respite Care I've just been reading about these two concepts for Alzheimer's care, which frankly could completely change the face of caregiving for families dealing with this difficult disease. Given that one of the biggest problems for family caregivers caring for their loved one at home is isolation/depression, the chance to be with a group of other caregivers (and care receivers) in an enjoyable social setting provided by the Memory Cafe is a perfect boost to mental and emotional health. Even respite care, though very necessary, doesn't provide the same kind of supportive, warm, interactive environment in which to simply exchange conversation, ideas and enjoy the company of others who completely understand the challenges of the Alzheimer's journey. It benefits both the caregiver and receiver to have this type of socially stimulating environment. It is not a "support group" for caregivers, since the aim is not to provide education, problem solving, or information, but rather just to have fun! The concept for Memory Cafes is really beginning to catch on in England, and is now being actively advocated here in the US as well. The focus is on positive reinforcement among peers, laughter, food and simple pleasure in the company of others who are going through the same journey -- without any stigma attached. After all, other caregivers will be much more understanding of behaviors that might cause embarassment in a public setting. According to John T. McFadden, in an article written for the Alzheimer's Reading Room: A Reminder: Why We Need Memory Cafes, "Memory Cafes are, first and foremost, a setting in which persons with memory loss can share fun and laughter with their care partners and friends in a setting free from awkwardness and stigma." Speaking as a former caregiver, I think this is a truly wonderful idea, one whose time has come! Mr. McFadden has written a newly released book to champion the cause, titled, Aging Together: Dementia, Friendship, and Flourishing Communities. He and his wife are planning to visit existing Memory Cafes in England in order to refine a model for use in America. This is a concept we should most definitely support. It just makes sense to tap this important resource we have in each other -- our sense of friendship and community, which can be an invaluable help to those on the front lines of Alzheimer's. The second concept, which is new to me, but has been practiced at the Hebrew Home at Riverdale in New York for the past 10 years, is overnight care for dementia patients to allow caregivers a good night's rest at home. This innovative concept makes 24-hour use of the nursing home facility, to provide day care from 8:30am to 4 pm and overnight care from 7 pm to 7 am. The program creates a sort of party atmosphere for the participants, with music, marimbas, and dancing as well as singalongs, crafts, and therapy sessions that last till dawn. There is also provision made for those whose Alzheimer's may be more advanced, which includes soothing sounds, aromatherapy, massage and touch therapy. If you would like to read more about this, here's a link to an Associated Press article appearing in the Wall Street Journal, updated October 1, 2012, titled: Overnight dementia 'camp' allows caregivers rest. Because so many Alzheimer's patients are very wakeful and sometimes agitated at night (called Sundowning), it creates major problems for families when their sleep is disrupted night after night by this behavior. Again, from a personal experience perspective, this was the single most insurmountable problem for my family -- sleep deprivation for months on end. It errodes a person's health, sanity, and makes the demands of caregiving impossible to continue. It is a major complaint of Alzheimer's caregivers and one of the main reasons for institutionalizing their loved one. It doesn't have to be if there are more programs for overnight respite care developed around the country. It really makes perfect sense to use facilities around the clock (with different shifts of staff, obviously), so that families can rest and resume their care duties after a good night's sleep. I would love to hear your feedback on these two concepts and any personal stories you'd like to share about how your family is affected by these challenges of caregiving. Feel free to comment below. 9/9/2012 Lessons from Alzheimer's, Part 1I found Alzheimer’s Disease to be a very powerful teacher over the course of my Mom’s 17-year journey through it. I want to share with you a couple of the most enlightening, soul-changing lessons it taught me:
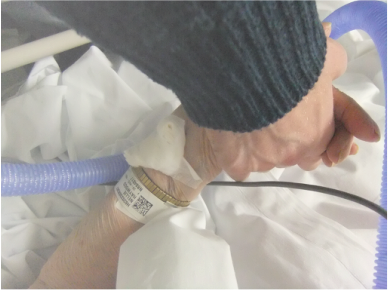
1.) Acceptance -- Alzheimer’s is a “kick in the gut” kind of disease. The diagnosis knocks the wind out of you like falling off a galloping horse and hitting the ground at great speed. It hurts like hell and leaves you bruised and aching. You have a visceral, deep, grief reaction, as if you’d been told someone you love died. And, in a sense, Alzheimer’s can be thought of as a very slow, mind-stealing, personality-altering thief of life. But it doesn’t have to be! When my mother was diagnosed, first I got very angry and railed at the Universe that such a sweet, wonderful person, who gave selflessly to others all her life, could possibly be punished with this affliction. Once I moved beyond that, I wanted to stick my head firmly in the sands of denial and keep it there for a decade or two. But I couldn’t. I had to help her through it. I had to accept what was -- reality. But I’m not talking about curling-up-in-a-small-ball-of misery-and-waving-the-white-flag-of-surrender kind of acceptance. No, indeed! What I’m advocating is a sort of life-affirming, defiant acceptance. The kind where you look fear (and Alzheimer’s) in the face and say, “I may not be able to stop you from taking precious pieces of my loved one, but you can’t take away our love, devotion, dignity and simple human pleasures of living. You can’t define who my mother is or who I am. You can’t take away the joy of being alive!” My defiant acceptance approach served us very well over the years. It gave me perspective on things and helped me navigate the very tough choices that had to be made on a day by day, sometimes moment by moment basis. Defiant acceptance allowed me to be not only the best advocate for my mother, but also the best daughter I could be. Both are vital. So, if you face a diagnosis of AD (I’m calling it AD from here on because it’s shorter to type), you can take the defiant acceptance approach, for yourself or your loved one. Cultivate the positive treasures of life, and wring every single drop of love and joy and satisfaction from each moment. It may not change the outcome, but it will make the journey rich, abundant, & beautiful beyond measure. Life worth living… 2.) Patience -- I don’t know about you, but for me Patience with a capital “P” has been a life-long lesson. Apparently, I’m a slow learner, so I’ve been given zillions of opportunities with this one! But Patience, like Acceptance, has many faces or facets. I found I was absolutely no good at sitting back in resigned silence, waiting for things to change or un-change back to what they were. I’m not that kind of person. I have way too much energy, passion and purpose for changing the world to be patient with injustice, with evil, with willful destruction of our planet, with man’s inhumanity to man, with greed, cruelty or unnecessary suffering -- all of which are crippling our world. So, in some circumstances at least, impatience is called for as a driving motivator for change, a call to action. Maybe I’m just trying to put my flaw in the best possible light :) But, be that as it may, I have lived my life learning patience over and over. Alzheimer’s Disease is a wonderful teacher of patience. Oh boy, is it ever! I had to learn to hear unlimited repetition -- of stories, of sayings, of poems, of songs, of questions, of observations -- I called this the endless-loop feature of AD. My Mom would just get “stuck” in an endless loop of repeating the same thing. For example, we were stranded in an airport after missing a connection (due to weather) and had a 5 hour wait for the flight home from a wedding. This was the last time I traveled with her alone by air. It had already been a very stressful trip. One in which my mother, as is common with AD, got very confused being in unfamiliar surroundings, out of her routine. I was sad that even while visiting the house where she was born and grew up, where her sister was still living, she remembered it not at all. So much for long term memory, I thought. So, as we were sitting in the airport (a place full of noise and commotion and distraction), I wasn’t able to leave her side, even for a minute--to get food, or tend to a call of nature. We were joined at the hip for five very long torturous hours. She must have asked the question, “Where are we going?” at least a thousand times. I’m not exaggerating. I started out telling her, in detail that we were going home from a wedding, I told her where we had been, whom we had seen, etc., but after the 248th repetition of this explanation, I got creative. Realizing that whatever I said wasn’t “sticking” in her brain, I just made up destinations -- like, Timbuktu, Crazy Wanna Come, Somewhere Over the Rainbow, and on like that. It became a kind of game, to distract her and keep me from going over the edge into insanity. It worked! It even entertained our seatmate on the plane, where Mom continued to ask the question and receive my very outlandish creative answers. It was harmless enough, and a rather good coping skill. But seriously, AD pushes anyone’s patience to the max. Even a saint might be sorely tried by the level of patience required 24/7/365. I’m not a saint (as those who know me will attest). But, I found the deep well of patience was there for me to draw upon in dealing with Mom’s condition, over and over, day after day, year after year. No, I wasn’t perfect, God no. I made mistakes. We all do. Here’s the big secret: as a caregiver, you don’t have to be perfect. You just have to be “there” and willing. That’s it! I just gave you perhaps the most valuable tool you’ll ever get -- you can forgive and be gentle with yourself. Your compassion for your loved one can spill over for yourself and that’s perfectly fine. So, try your hand at practicing Creative Patience, or Selective Patience, and see how it changes your inner self and eases the journey. I’ll continue these Lessons from AD in future blog posts. Stay tuned for more action and adventure on the journey of care giving! 9/6/2012 Caring in the HospitalOne of the most challenging caregiving experiences can happen, ironically, when your loved one is admitted to someone else's care: ie. the hospital, rehab or nursing home. In my own 17-year caregiving journey, my mother was only admitted to a hospital three times, two of those during the last 7 months of her life. Each time it was very traumatic (for both of us!), but what I found so stupefying was the total inconsistency of the quality of care. The difference was dramatic, both from hospital to hospital and even from floor to floor of the same hospital! It covered the whole spectrum between basically decent to almost criminally negligent. From these experiences, which I will not share in gruesome detail, I found three nuggets of truth to be evident:
1) Hospitals are not good places for the elderly, and are especially bad for those with any type of dementia. Anytime someone is in pain or physical distress, it clouds their thinking capabilities, and if drugs are given, they can intensify this effect. Same goes for the changes in routine, unfamiliar surroundings and upset in sleep patterns that happen in hospitals. In fact, according to a recent study, a hospital stay can actually be a causal factor, triggering dementia in the elderly, if delirium is present during the hospitalization. The article in Science Daily explains the long-term effects and also gives some ways to help avoid delirium and consequent cognitive decline: Delirium and Long-Term Cognitive Decline in Alzheimer's Patients Linked in New Study http://www.sciencedaily.com/releases/2012/08/120820161009.htm So, for the sake of all concerned, take whatever steps are possible to minimize or altogether avoid hospital admissions. For example, during one emergency, I waited with my mother for over 5 hours in the hospital ER waiting room, only to find there were still several people (and hours of waiting) ahead of us. Because I knew Mom was in a weak and debilitated condition, getting worse by the minute, I called the local walk-in clinic. They had no one waiting, took her in within two minutes of arrival, examined and treated her in less than an hour. She improved dramatically by the following day, when I was able to get her in to see her regular doctor. We thus avoided what would have likely been an unnecessary hospitalization. That was a very valuable lesson. Obviously, you have to use best judgement as to the severity of the problem. It's always best to call 911 if you have a true life-threatening emergency, but consider the risks against the benefits for less threatening circumstances. Another time, we waited over 11 hours in the emergency room, much of it with me sitting on a cold hard floor next to her gurney because they didn't "allow" family to be in there. I had to explain repeatedly that her mental status required my presence, since she couldn't answer questions or give a medical history. They eventually brought me a chair when they realized I wasn't going away, no matter what they said. (This was less an act of kindness than that they just got tired of tripping over me). This marathon ER experience happened in 2003, and I truly hope that hospital staff has become more aware of and sensitive to the needs of elderly dementia patients to have their caregivers present in these very upsetting and frightening situations. 2) The elderly are at risk for falling in many cases, and that risk increases when they are in a hospital setting. In fact, my mother's first fall, after living with us for nearly 8 years without a mishap, was when she was in the hospital. She was disoriented, on IV and yet managed to get out of bed to try to get to the bathroom on her own. She fell, but thankfully was only banged up a bit and didn't suffer any major trauma or broken bones. It was a wake up call for me! So, my advice would be to stay with your loved one as much as possible, and if you can afford it, hire extra care so that someone is in attendance when you cannot be there. If you can't afford this (it's quite expensive!) you can arrange for friends, church members, and/or other family members to volunteer so that there is adequate coverage. You will need to see to personal hygiene, such as brushing teeth (or cleaning dentures), shaving, putting in and removing hearing aids, and sometimes even bathing your loved one, depending on the staff (or lack thereof) in the particular facility. But don't expect the care to just happen. It won't. Doing it yourself insures that your loved one's basic needs are met and they can be comfortable. I also believe it helps them tremendously to remain "in touch" with you, quite literally. 3) And lastly, do whatever you must to "catch" the doctor while making rounds. Be sneaky, lie in wait. This may require being in the hospital room by 7 am or earlier, since many doctors do rounds before starting an office schedule. Ask the nurses what time a doctor normally sees patients and make your ambush plans accordingly. You want to communicate, question, understand treatment plans and diagnosis/prognosis. A new trend in so-called "care" involves having a "hospitalist" -- a doctor that is specifically assigned from a practice to care for all hospitalized patients from that practice. This makes absolutely no sense, since the attending physician may know nothing about the patient, having never seen them prior. If there is dementia or even just normal disorientation resulting from the injury or illness requiring hospitalization, the patient can't give vital information to assist with treatment or diagnosis, nor can they, in the case of Alzheimer's, even answer the most basic questions. This becomes downright dangerous to the patient, and I'm sure is frustrating for the doctor, too. Hence my advice to lie in wait if you have to, in order to ask questions and interact with the doctor in person. It is my firm belief, after witnessing some harrowing hospital horrors, that everyone needs an advocate to intercede on their behalf. As an advocate, you need to be very clear and specific in asking about any drugs that are being given, or considered, and what the risks vs. benefits are, as it can be a devastating ordeal if inappropriate medications are ordered. Case in point: Anti-psychotic drugs, such as Haldol (halperidol) are all too often given to Alzheimer's patients with sometimes deadly results. I have personal experience of this with two elderly relatives. The consequences were tragic. There is an excellent blog post on this very subject at the Mayo Clinic Alzheimer's Caregiver Newsletter, which I will share here: http://www.mayoclinic.com/health/antipsychotics-and-alzheimers/MY02213/ Forewarned is forearmed, though it is such a shame to have to think of a hospitalization in terms of doing battle. Unfortunately, that is often the true nature of care in our present system. To be fair, there are still a few rare, white knights disguised as doctors, riding in with the best ideals, and highest standards. But, they are sadly more fictional than real these days. If you are fortunate enough to find one of these very special health care professionals, give thanks, hold on and don't let go! |
About Karen
Karen is a compassionate, enthusiastic student of life, who cared for her mother for 17 years. She brings her insights, compassion, experience and desire to share knowledge and healing to this ongoing conversation with others on the caregiving path. If you are caring for a parent, spouse, friend or other loved one this site offers sanity-saving tips, open-hearted self-care ideas, and an open forum for discussion, connection and sharing resources for the journey. Archives
October 2021
CategoriesAll Acceptance Aging Together Alan Cohen Alive Inside Movie Alzheimer's Alzheimer's Prevention A Mind Of Your Own Anxiety Aromatherapy Audio Therapy For PTSD Austin Air Hepa Filter Autism Back Care Video Beginner's Mind Being Present Blessing For Caregivers Books Brain Insulin Butterfly Story Calm Calm.com App Care For Veterans Caregiver Advocate Caregiver Coalition Caregiver Comfort Kit Caregiver Guilt Caregiver Retreat Caregiver's Serenity Prayer Caregiver Stress Caregiver Support Care Giving Caregiving Vulnerability Care In Hospital Caterpillar Into Butterflies Chamomile Tea Cindy Laverty Comedian Computers & Exercise Crisis Dan Cohen Deepak Chopra Delirium Depression Diabetes Disaster Preparedness Distractions Dr. Dharma Singh Khalsa Dr. Oliver Sacks Eden Alternative Eldershire Elizabeth Dole Foundation Emergency Planning Emergency Preparation Emerson End Of Caregiving Enough Already Escapism Essential Oils Food Safety Forgiveness Funny Stories Gaiam.com Gail Sheehy Gift Of Alzheimer Gift Of Healing Presence GMO Food Green House Project Gregory Fricchione Md Grief Guilt Happy Light Healing Holding Hands Home As Sanctuary Hope Hospital Caregiving Hospital Stay Humor Inspirational Reading Ipods For Nursing Homes Isolation Jacksonville James E. Miller John Denver Johns Hopkins Study John T. McFadden Jon Kabat-Zinn Kelly Brogan Kirtan Kriya Meditation Lao Tzu Laugh Laughter Lavender Loneliness Loss Of Purpose Love Love In The Nursing Home Maya Angelou Mayo Clinic Mayo Clinic Alzheimer's Blog MD Meditation Meditation Garden Melatonin Memory Memory Cafe Military Caregiver Mindfulness Meditation Mr. Bean Music Music & Alzheimer Music And Memory Neurological Research Noise Pollution Operation Family Caregiver Opportunity Overnight Respite Care Pandemic Passages In Caregiving Patience Paul Coelho Peace Post-traumatic Stress Disorder Power Of Love Prayer PTSD Quality Of Sleep Radical Contentment Relaxation Releasing Problems Renewal Research Respite Rewind Rodney Yee Rosalynn Carter Rosalynn Carter Institute For Caregiving Rowan Atkinson Sanctuary Sanity Self Care Serenity Silence Sleep Slowing Time Solutions Soothing Music Stress Stress Relief Sun Sunshine Support For Caregivers Tai Chi Thanksgiving The Care Company The Kiss Time Traumatic Brain Injury Travel With Alzheimer's Person Treat VA Caregivers Valentine's Day Verilux Veteran Farms Veterans Veteran Suicide Vitamin D Wayne W. Dyer Wellness Wendell Berry White Noise William H. Thomas Worry Yoga Yoga Video |
Caregiver Wellness
Popular pages on this site:
|
Self-Care Practices
Explore what works for you:
|
Original content © 2012-2023 Karen Bonnell all rights reserved